Prof. Dr. Robert Hierner at a glance.
FAQs for Scar Removal in Dubai
The request for scar treatment is increasing in importance today. Pioneered by a few experts like Prof Dr Robert, Scar Care is a special interdisciplinary treatment that includes other specialist such as dermatology, physiotherapy, radiotherapy, mental health, anaesthesia, cosmetology and hand surgery to treat as kind of scar optimally.
Do scars ever go away? Are scars permanent?
Your scar might itch for a number of reasons. As your wound heals itching is a healthy sign of the healing process. It is very tempting to scratch at your wound, but ill advised as it might make your scar appear worse. Some scars continue to itch for a long time after they have healed. This can cause severe discomfort. It is thought that the reason for your scar itching is linked to the damage done to nerve endings around the wound. If your scar stretches then they will be irritated, and are likely to itch as a consequence. If your scar itches it is best to ask the advice of your GP and to ensure that it is not because the skin is dry. Using a good moisturiser can help to ease any itching of the skin.
How long will it take for the scar to heal after injury/surgery?
The healing process varies depending on the individual and the reason of injury. While initial healing may occur within a few weeks, it can take several months to a year for a scar to fully mature and for the final results to be visible. Patience and following aftercare instructions are key to a successful outcome.
What is scar revision surgery?
Scar revision surgery is a specialised procedure aimed at improving the appearance of scars. This type of surgery seeks to minimise the scar so that it is more consistent with the surrounding skin tone and texture. It can be performed on any part of the body and is tailored to the individual needs of the patient, taking into account the type and severity of the scarring.
Can scar revision surgery completely remove a scar?
While scar revision surgery can improve the appearance of a scar, making it less noticeable or more easily concealed, it is important to understand that it cannot completely erase a scar. The goal of the surgery is to make the scar less prominent and more similar in texture and colour to the surrounding skin.
How long should I wait after the initial injury or surgery before considering scar revision?
It’s often recommended to wait at least a year after the initial injury or surgery before considering scar revision, as scars can naturally improve in appearance during this time. Some scars may require more time to mature, and waiting allows you to see the full extent of the scar’s development before making a decision.
What is the recovery process like after scar revision surgery?
Recovery varies depending on the surgical technique used. You may experience swelling, redness, and discomfort in the treated area. Detailed post-operative instructions will be provided, including how to care for the wound, signs of infection to watch for, and when to return for follow-up appointments. Recovery time can range from a few days for minor procedures to several weeks for more extensive surgeries.

Ask the Expert about Scar Removal.
Prof. Dr. Robert Hierner offers specialized scar removal treatments in Dubai, utilizing interdisciplinary approaches to enhance skin appearance and address both physical and psychological impacts of scarring.
Scar Removal - Procedures
Scar Suppression (Fresh Scar Treatment)
Fresh Scar treatment is possible during scar maturation, a process that usually takes several months. The principle applies “As long as a scar is red, it can be improved”.
There are various simple, conservative therapy options to influence scar maturation, these are summarized in the so-called "Scar Suppression Ladder".
1. Basic Skin Care
The quality and moisture condition of the skin has a decisive influence on scar formation.
Skin care with refatting crème (Vaseline, Mebo Scar, etc.) 3 – 5x/day by the patient.
2. Scar Massage
The massage is crucial, not the ointment.
Scar massage with refatting crème (Vaseline, Mebo Scar, …) 3 – 5x/day by the patient.
Goals of treatment are:
- Desensibilisation (reduction of hypersensitivity)
- Reduction of scar volume
- Reduction od scar redness
Removal of scar adhesion.
3. Edema/Swelling Management
Adequate Edema Management speeds up wound healing and scar maturation.
Compression-Therapy on a scar leads to a so-called “beneficial ischemia”. Depending on the mount of pressure there is:
- Acceleration of scar maturation, if > 15 mmHG
- Reduction of scar volume, if > 25 mmHG
4. Silicone Sheet therapy
Silicone sheet therapy is a cornerstone of successful scar suppressive treatment
Application of a thick silicone sheet on a scar has an occlusive effect and leads to a local increase of temperature and water steam, which are thought to be the main responsible changing that:
- Reduce scar redness
- Improve scar suppleness
5. Combined Silicone and Compression Therapy
Combined Silicone and compression treatment lead to an amplification the effect of the individual components
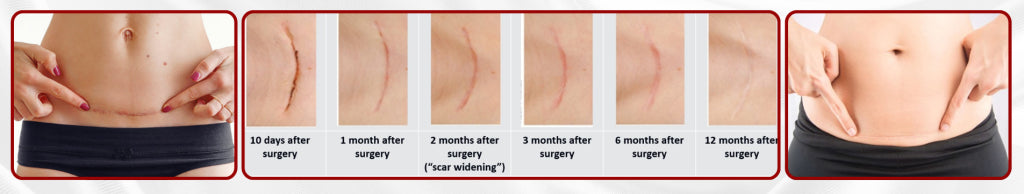
Silicone Sheet Treatment
Based on the positive experience in burn patients, silicone therapy became a well-accepted standard treatment in burns. When transferring this treatment method to other scar types such as surgical scars and keloids, some key points need to be discussed in detail with the patient.
When to start Silicone Treatment?
Silicone Therapy can only be started after complete wound healing, which is about 2 – 3 weeks after injury/surgery.
Should I use a silicone patch or silicone gel?
Whenever possible, the silicone platch should be used, as it has a significantly higher scar-suppressing effect than the silicone gel.
Silicone gel is only indicated when a silicone patch cannot be used (e.g. face).
How to apply the Silicone Sheet on the Scar?
For adequate scar therapy it is necessary that all edges of the silicone patch are at least 1 – 1.5 cm away from the scar.After planning the size of the silicone patch, this can be cut off the large piece of silicone with regular scissors. Before the silicone plaster can be applied, it must be checked that there are no residues of creams on the skin. The Basic Skin Care and Scar Massage with Fat cremes must always be carried out after the silicone plaster has been removed.
What do you have to consider when starting therapy?
At the start of therapy, care must be taken to gradually adapt the skin to the new conditions in order to avoid possible side effects.
Each silicone therapy starts with a duration of 2 hours. During the first week, the duration of therapy is increased by 2 hours per day. If redness with itching occurs in the area of the silicone plaster, the treatment must be interrupted for 24 hours and then continued with the same therapy duration.
How many hours a day should you wear silicone scar sheets?
We recommend wearing the sheets for 12 to 20 hours, making sure you remove them daily to allow the area to be washed, cleaned and refatted. Silicone patches can be worn during night time or during day time, depending on the patients`activities and the preferences.
How long can you use one Silicone Patch?
The same silicone patch can be used for 4 – 6 weeks, provided good maintenance. The silicone patch should be changed when it loses its self-adhesive function.
How do you wash Silicone Scar Sheets?
Silicone sheets should be cleaned daily to maintain adhesive strength: Rub the sheet with a few drops of cleaning soap or neutral soap and lukewarm water. Rinse the Silicone sheet well under lukewarm, running water so that all dirt and soap residue is removed. The washed silicone plaster should be placed on the edge of the sink or on a smooth surface with the non-stick side down.
How long does the whole Silicone Therapy last?
In the course of scar maturation, the scar changes color. The principle applies: “As long as a scar is red, it can be improved by silicone treatment. For most patients a period of 3 – 6 months is necessary".
How often do I have to go to Scar Check-ups?
Follow-up examinations at the following points in time have proven effective in scar therapy:
- 3 weeks post-op (start scar treatment)
- 6 weeks post-op (control swelling, control scar treatment)
- 12 weeks post-op (control swelling, control scar treatment)
- 1 year post-op (long term result)
Does silicone therapy rid of scars?
Silicone therapy does not lead to scar removal, but to an improvement in the appearance of scars in most patients.
What are the Benefits of the Silicone Therapy?
The application of a silicone patch helps soften, flatten, and fade scars, by:
- Reduction of Scarring, thus improvement of scar soupleness
- Acceleration of maturation process, thus earlier reduction of scar redness
What are the Risks of the Silicone Therapy?
Silicone treatment is a safe procedure. There have been no reported side effects from using silicone strips because it is made of non-toxic, medical-grade silicone.
In rare cases, very sensitive skin may experience redness and itching in the area of the silicone plaster at the beginning of the treatment. In this case, silicone therapy should be stopped for 24 – 48 hours and then restarted.
What are the costs of the Silicone Therapy?
Silicone patches can be purchased at the pharmacy or online. Depending on the quality of the silicon patch, the price varies from 40 to 260 AED.
C-Section (Correction of surgical Scars)
If a scar is established, there are multiple conservative, minimal-invasive (Peeling, LASER, Dermabrasion, Filler (Hyaluronic acid), Fat transfer, Stem cells ) and operative treatment options to improve it. Very often several treatment option are used in combination. The choice of treatment option(s) is determined by the type of scar
There is a high rate of patient satisfaction . But keep in mind that the scar healing process takes about a year. Scars typically start out as red, then tighten, and finally relax into a more subtle color. The patient has to participate actively in the scar suppression treatment (→ fresh scar treatment). The skin above the surgery area may be slightly less sensitive for 1-3 months.
Conservative Treatment
Scar massage is the basis of each and every scar treatment. There are different techniques delivered by physiotherapy
Goals of the scar massage are:
- Desensibilisation (reduction of hypersensitivity)
- Reduction of scar volume
- Reduction od scar redness
- Removal of scar adhesion
The massage is crucial, not the ointment“: Scar massage with refatting crème (Vaseline, Mebo Scar, e.t.c.) 3 – 5x/day by the patient.
Minimal-invasive Treatment
Correction of the scar surface is mainly done with any kind of skin-resurfacing techniques techniques such as
- Peeling
- Laser
- Dermabrasion
Surgical Treatment
Correction of the scar width, pattern, course and scar contracture can only be achieved by surgical scar correction.
- Scar excision & Plastic-surgical skin suture
- Scar excision & shifting the course of the scar
- Scar excision & Tissue Transplantation
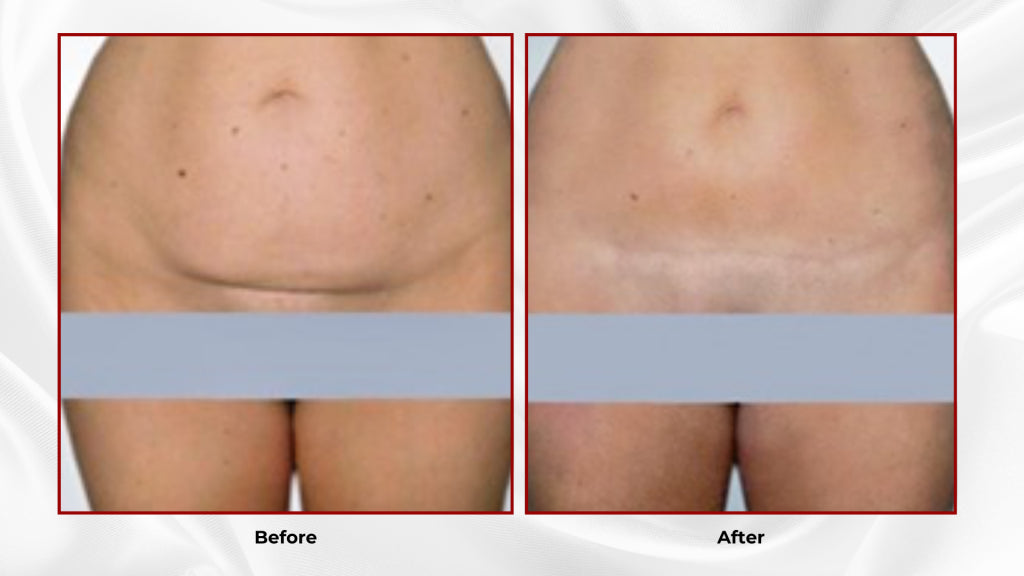
Keloid - Procedures
A Keloid scar is a thick (hypertrophic) scar above skin level that grows beyond the initial wound area and frequently shows itching. It usually forms on earlobes, shoulders, cheeks or the chest. There is a strong genetic background.
Goals of treatment
Goals of treatment are:
- Stop/Reduction of itching
- Stop scar growth
- Improvement of scar shape and color (optional)
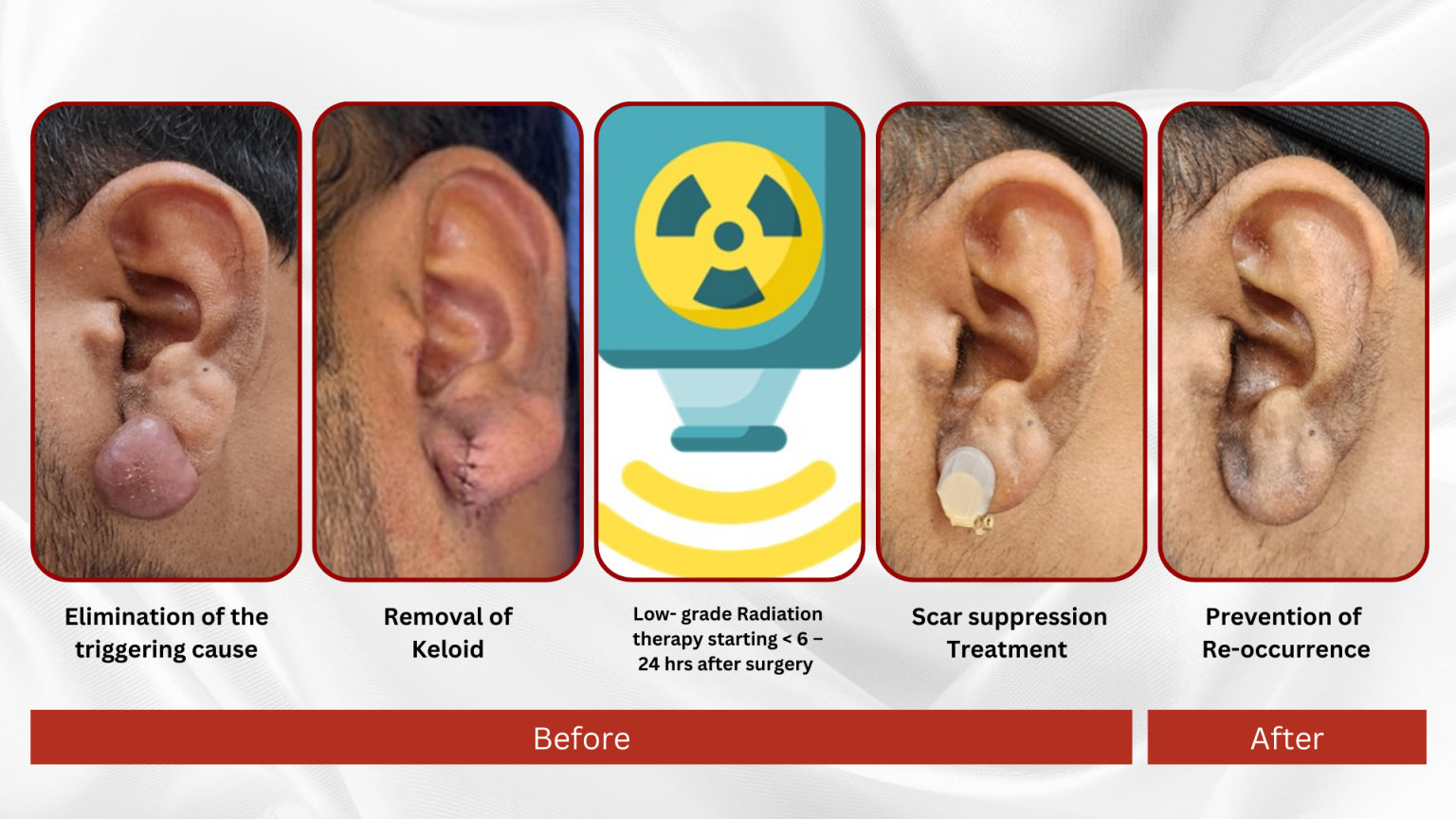
Regardless of the method chosen there are always 4 steps:
- Elimination of the triggering cause: Every treatment starts with the elimination of the triggering cause (e.g. earrings, pearcing, …)
- Removal of Keloid: Depending on the size of the keloid, there are different treatment option:
- Combined Keloid Treatment: Keloid Resection and postoperative Low-Dose Radiotherapy (LDRT) < 6 – 24 h (see below)
- Scar suppression Treatment: (→ link Fresh Scar treatment (Scar Suppression)
- Prevention of Re-occurrence: Adequate postoperative scar management is crucial and comprises scar compression treatment in combination with silicon sheet application until redness of the scar subsides (6 – 12 months).
NOTE: Most Keloid treatment show a high recurrence rate (80 – 90 %). To effectively avoid a recurrence after treatment keloid, it is necessary to combined several treatment options.
Keloid Resection and postoperative Low-Dose Radiotherapy (LDRT) < 6 – 24 h
If surgery is necessary it should always be combined with postoperative Low-Dose Radiotherapy (LDRT) within the first 6 to 24 hrs after surgery, in order to reduced early wound healing cascades and lower the recurrence rate to 5 – 10 %.
How is a patient for Low-grade radiotherapy?
All patients, who suffer severe keloid at the earlobe, or recurrence after minimal-invasive keloid treatment (cortison injection, cryotherapy) can be treated with low-dose radiotherapy (LDRT) as an essential part of multimodal treatments.
Prof. Dr. Robert Hierner, a renowned scar specialist in Dubai, will examine keloid and symptoms, and suggest the treatment.
Low-Dose Radiotherapy (LDRT) is one of the pillars of therapy in the multimodal treatment of keloids
What is Radiotherapy and how is it effective for keloid treatment?
Low-dose radiotherapy is a therapeutic tool for treating all proliferative diseases of the soft tissues. Keloid is a hyperproliferating scar. Hence LDRT treatment can help in alleviating keloid symptoms.
Where can Low-dose Radiotherapy (LDRT) for keloid treatment be done ?
Low-dose Radiotherapy (LDRT) for keloid treatment is carried out at the Department of Radiotherapy (Head: Dr. Osama Aldabass) of the Saudi German Hospital Dubai.
Acne Scars
While for most patients, acne heals completely without leaving scars, for others these are a lasting reminder of the skin disease.
If the course of the disease is particularly severe, scars can characterize the skin and become a psychological burden for those affected.
The following basic principles have proven effective:
- The best treatment of Acne scar is prevention
→ early onset of adequate local and systemic acne treatment
- If acne scars cannot be prevented, the must be treated early
→ reduce/stop of any residual acne disease activity (→ Dermatology)
- Once acne scars are established, the aim is to make them less noticeable
→ rule out any residual acne disease activity before starting invasive local scar treatment (reduction of infection risk).
→ Lines of treatment (Subcision, LASER, injections, Biostimulator, Peeling, Microneedling, Plasma, Growth factors, Stem cell, fillers, fat injection, RF)
Note: in severe cases autologous fat cell transfer (Lipofilling) has proven a reliable method to significantly improve the appearance.
Skin-resurfacing
Compensation of unevenness by “thinning” the skin down to the superficial dermis with spontaneous regeneration. Procedures need to be repeated 2 – 3 times with a minimal distance of 6 – 12 weeks.
- Peeling
- Laser
- Dermabrasion
Scar Release (Subcesion) & Fat grafting
In severe cases autologous fat cell transfer (Lipofilling) has proven a reliable method to significantly improve the appearance. The treatment is divided into 3 steps:
- The liposuction for harvest of fat graft is performed under local anesthesia, if desired also combined with a light twilight sleep. The main donor region is the inner thigh (one surgical field). After suctioning, ensure adequate wound drainage. A highly absorbent bandage is applied.
- Scar release (subcision) is also carried out under local anesthesia.
- The fat transfer (autologous fat injection, lipofilling) Then a certain amount of autologous fat is inserted into the respective skin layer with a fine needle. Small dressing (Steristrip) may be necessary in rare cases.
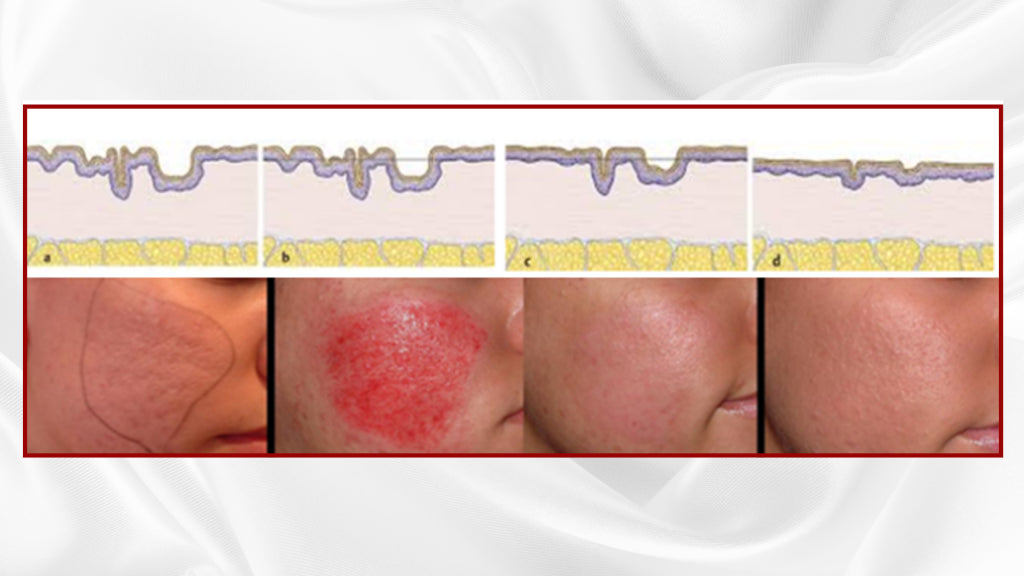
Stretch Marks
A stretch mark is a type of scar that develops when our dermis ruptures. Dermis rupture is likely to occur, when:
- family disposition
- periods, were our skin stretches quickly (i.e. growth spurts in puberty, pregnancy, rapid weight gain)
- in case of high cortisone level for longtime (medication, Cushing disease, …)
There are several treatment option available. It’s important to understand that no single treatment works for everyone — and many products don’t seem to work at all. The following basic principles have proven effective:
- The best treatment of Stretch marks is prevention
- If stretch mark cannot be prevented, the must be treated early

Burn Scars
Burn scars are thick (hypertropic) scars covering the area of the burn injury with a scar plate:
- Treatment of fresh burn scars
- Treatment of old burn scars
- Treatment of scar contracture
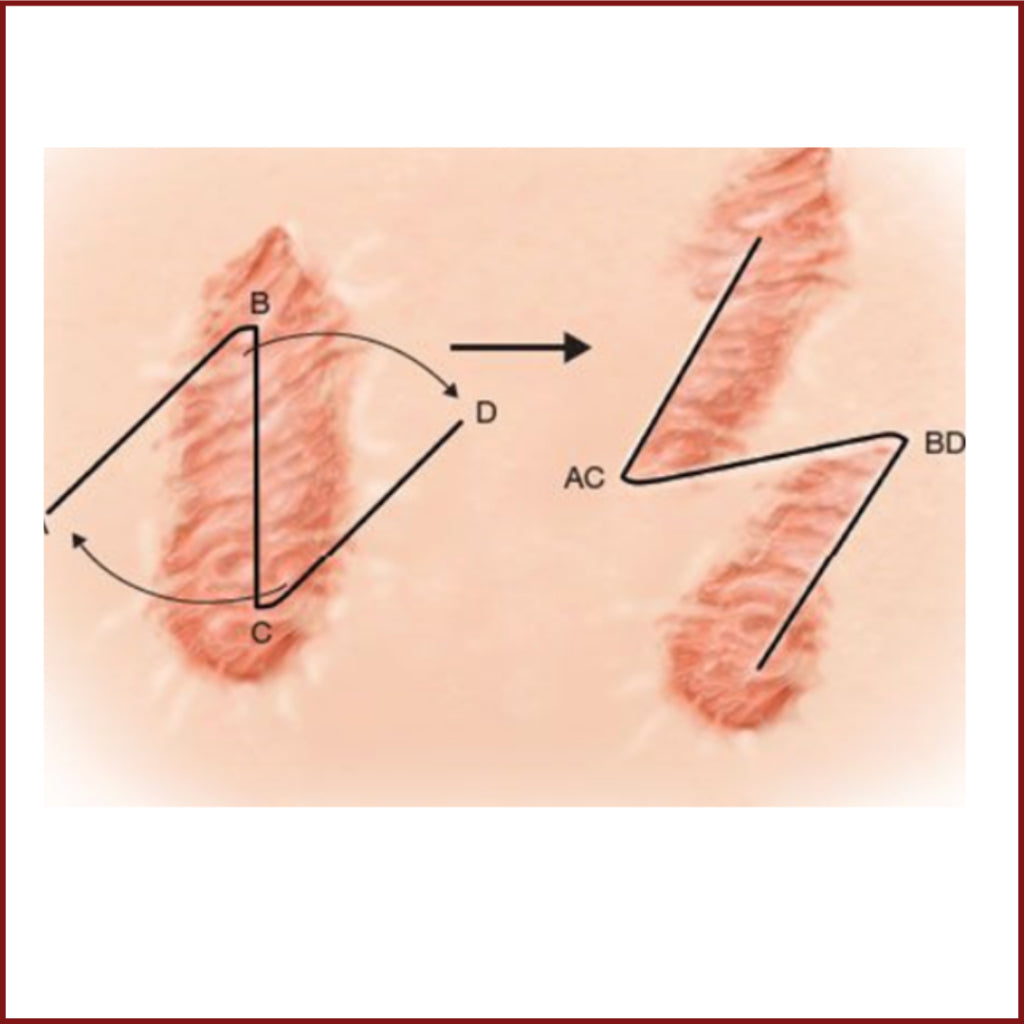
Scar contractures are functionally more important the closer they are to a joint and the more perpendicular they are to the Skin Lines. Basic principles of surgical scar correction are:
- Interruption of the scar by inserted tissue
- Change in the course of the scar (parallel to the skin tension lines).
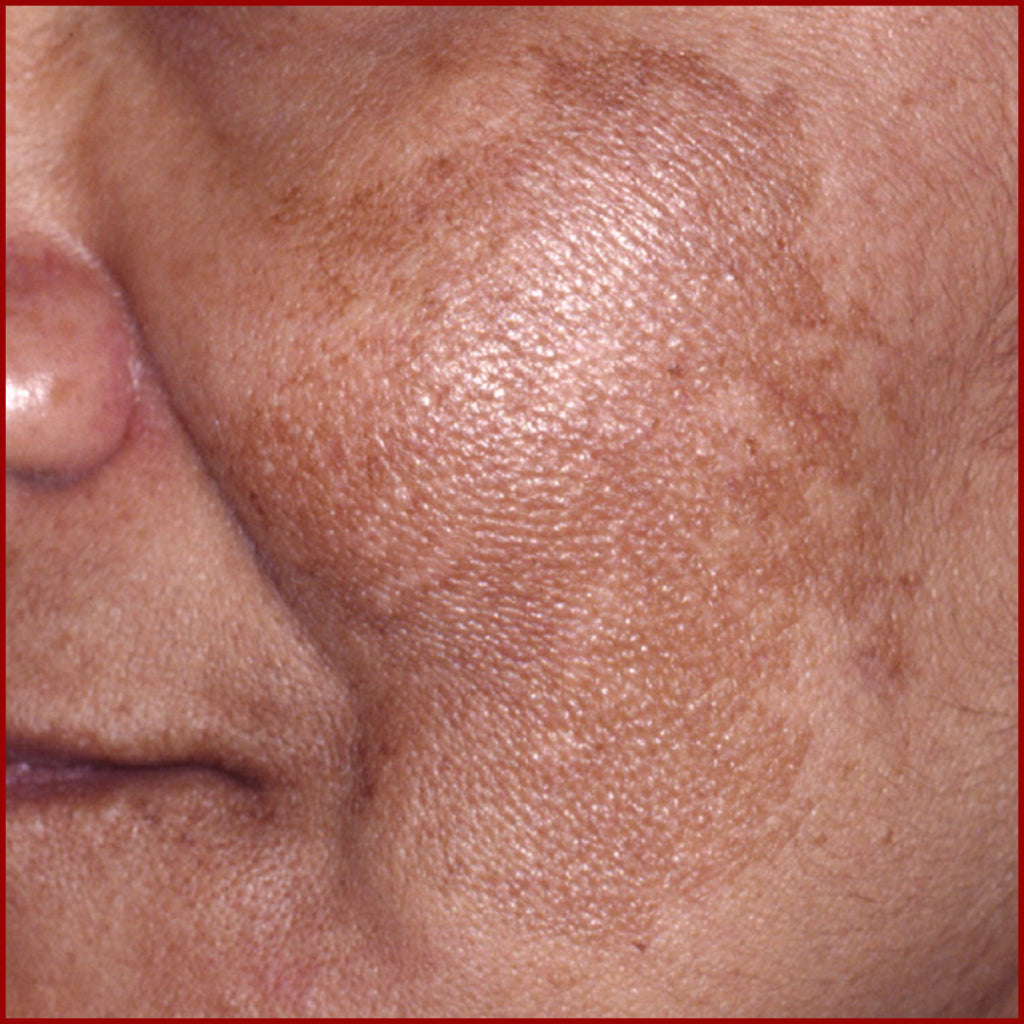
Color (Pigmentation) Disorder
Pigmentation problems are a common consequence of deep partial- and full-thickness burns, other skin trauma, and surgical procedures. Altered skin pigmentation in scars, can result from increased or decreased pigment (melanin), abnormal pigment (melanin) distribution, or deposition of exogenous substances.
In principle, a distinction is made between too much skin pigment (hyperpigmentation) and too little skin pigment (hypopigmentation). In scars, both conditions often occur at the same time.
Both hypopigmentation and hyperpigmentation can cause esthetic and psychological issues, which may influence quality of life.
Too much Color (Hyperpigmentation)
- Stop Squeezing and scatches (e.g. Acne)
- Sunscreen
- Topical whitening (use combined treatments)
Too few (Hypopigmentation)
Some scars can no longer be improved by any conservative and surgical measures (e.g. pigment changes). Appropriate scar cover can make these scars appear less noticeable.
Temporary Scar covering
Temporary Scar covering is indicated at any point in the scar therapy, it is at the beginning of every scar therapy and is at the same time the icing on the cake of a successful scar therapy. There are 2 main options:
- Camouflage is used up in areas, in which conspicuous color differences need to be “covered up”
- “Corrective make-up” is and advanced form of camouflage used at the face. With the help of a few practical make-up tips, pigment changes can be concealed, and the patient’s social acceptance can be significantly improved
Permanent Scar Covering
Permantent scar covering by micropigmentation (tatooing) is routinely done by medical tattoo artist in oncological breast reconstruction patient for the nipple reconstruction. In Scar treatment there are 2 main option:
- Discretion, i.e. try to even out the color difference (→ skin micropigmentation)
- Distraction, i.e. try to cover up the scar with a tattoo
Soul Scars
“Body and Soul”: Tissue damage not only leads to an externally more or less visible scar (Body Scar) but often also to psychological trauma (Soul Scar).
“Stress and Coping”: The reality of a serious physical illness (cancer, transplant, stroke, etc.) leads to extreme human situations that the sick person, their family and their psychosocial environment have to cope with.
The task of medicine is to keep the sick not only “alive”, but also “in life”.